According to the Centers for Disease Control (CDC), more than 37 million people in the United States are living with diabetes. That’s over 11% of the population. With another estimated 96 million diagnosed with prediabetes, diabetes is one of the top chronic diseases facing us today.
What exactly is diabetes?
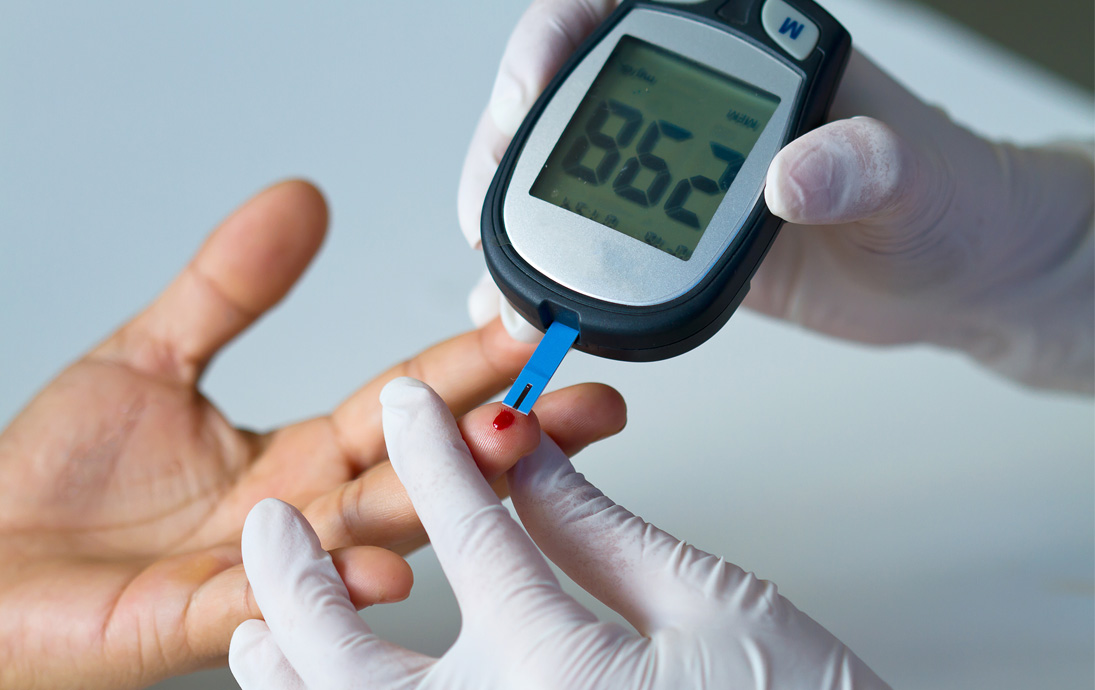
Diabetes is a chronic health condition that affects how your body turns food into energy. As your body breaks down the food you eat into sugar, it then releases into your bloodstream. When your blood sugar increases, your pancreas is signaled to release insulin.
Diabetes develops when your pancreas doesn’t make any insulin, makes too little insulin, or when your body doesn’t respond to the insulin properly.
Diabetes affects people of all ages and is manageable with medications and/or lifestyle changes. While each individual should work with their doctor on their specific treatment plan, often times, medications may be prescribed to help manage this disease. One of the most prevalent medications for diabetes is insulin.
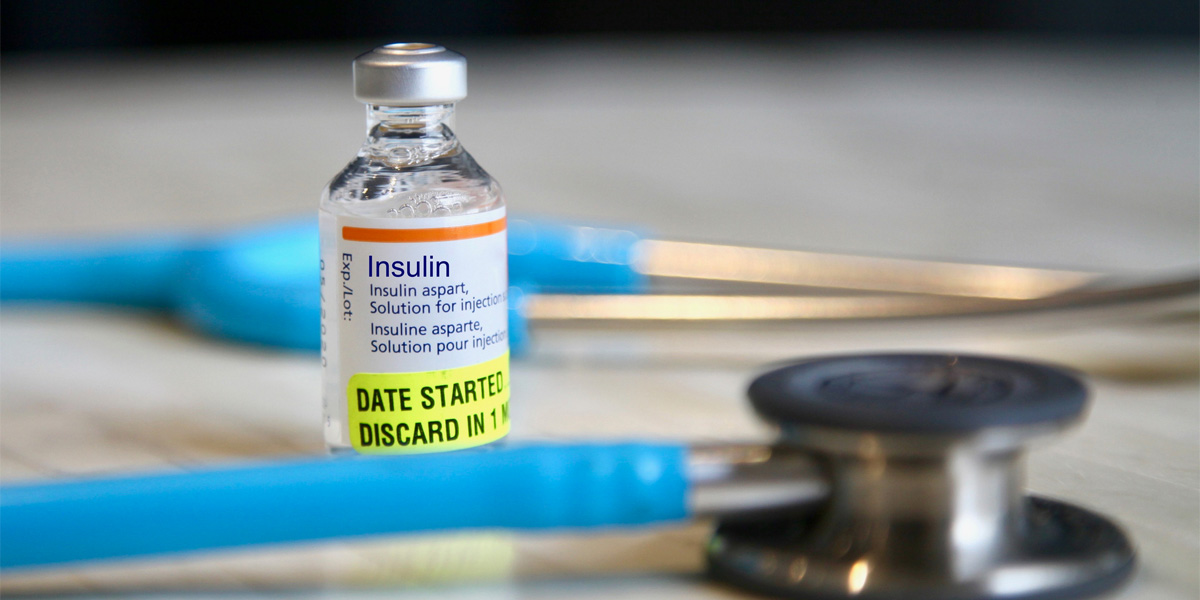
Let’s talk about insulin
Insulin is an essential hormone that helps your body turn food into energy and controls your blood sugar levels. Think of your body as a car, and food as the fuel that makes the car go. Insulin is like the key that unlocks the fuel tank and lets the fuel (or food) into the engine (or your cells).
When you eat food, your body breaks it down into smaller parts, including a type of sugar called glucose. Glucose is important because it's what gives your body energy to do every day activities. But glucose can't get into your cells on its own, it needs insulin to unlock the door.
So, when you eat, your body releases insulin into your bloodstream. The insulin tells your cells to open up and let the glucose in, where it can be turned into energy.
Some people's bodies, however, don't make enough insulin on their own, or their cells don't respond to insulin the way they should. If your body isn’t able to produce enough insulin, a doctor may prescribe human-made insulin as a diabetes treatment. Insulin comes in many forms, including an injection (shot), injectable pen or pump, and also an inhalable insulin powder.
The impact of increasing insulin costs
The rising cost of diabetes largely tracks with the dramatic increase in the cost of prescription insulin. NPR.org reports that the price of insulin has increased by more than 600% over the last 20 years and studies conducted by the American Diabetes Association find that one in four people that use insulin report rationing their insulin supply because they cannot afford the cost of their full prescribed dosage. Researchers at Yale also found that 14% of people who use insulin in the United States face what are described as “catastrophic” levels of spending on insulin, meaning they spent at least 40% of their post subsistence income (what is available after paying for food and housing) on insulin.
Rising insulin prices and the resulting rationing or missing doses of insulin can have severe consequences for diabetics. Many are often forced to make a choice between insulin and other health-related services or other bills like housing and utilities. If left untreated, diabetes can lead to devastating complications, such as heart disease, nerve damage, blindness, kidney failure and amputations. And the risk of death for adults with diabetes is 50 percent higher than for adults without diabetes.
Positive movement to affordable insulin
In August 2022, Congress passed the Inflation Reduction Act which capped insulin copays at $35 per month for people with diabetes on Medicare. With pressure from the federal government, several manufacturers then announced price reductions or price caps for out-of-pocket insulin costs in 2023.
Additionally, bipartisan legislation was introduced in Congress in April 2023, the Improving Needed Safeguards for Users of Lifesaving Insulin Now (INSULIN) Act of 2023, which is an effort to comprehensively tackle the skyrocketing costs of insulin, removing barriers to care, and making insulin more accessible for millions of Americans. This legislation aims to address structural issues in the insulin market, create policies to foster more competition and expand access to insulin medications.
Good news for PHP members! Zero Cost-share Insulins.
PHP members have access to many preferred insulin products on the PHP drug formulary with no out-of-pocket cost.
“We don’t want to see patients who require insulin miss their doses because they can’t afford it, but we know that can happen because of the high cost of insulin,” said Nick Sloffer, RPh, PHP’s Director of Pharmacy. “At PHP, three of our top six highest cost drug categories are for the treatment of diabetes. By making insulin more affordable, we know we can help members achieve the best health outcomes and avoid the more severe and advanced health issues that arise from untreated or undertreated diabetes.”
This pharmacy program includes the most-used insulins by our PHP members, and results in significant savings for those currently using these products. The no cost-share preferred insulin products includes various dosages and forms of: Humalog, Humulin, Insulin Lispro, Lyumjev, Semglee, Soliqua, Toujeo, Tresiba, and Xultophy.
Members with additional questions can contact PHP Customer Service at custsvc@phpni.com, 1-800-982-6257, or via online chat at www.phpni.com.